
Why Surgery Before Age 7 Changed My Brain Forever
I was four years old when I had my first hip surgery.
I was four years old when I had my first hip surgery.
Four years old when I learned that my body could be a source of pain. That adults could hurt me even when they were trying to help. That screaming didn't make it stop.
Four years old when my brain was still forming the foundational beliefs about safety, trust, and whether the world was a place I could relax in.
And that timing? It matters more than anyone told my parents.
Because when trauma happens before age seven—when your brain is still developing its core understanding of the world—it doesn't just create memories. It shapes the architecture of your nervous system.
I didn't know this for 30 years. I thought I was just broken. Sensitive. Unable to cope with normal life.
Turns out, my brain was doing exactly what trauma brains do when the wiring gets installed during fear.
The Brain Science No One Explained to Me
When I read The Body Keeps the Score by Bessel van der Kolk, I had to pull over while walking and just stand there.
Because he was describing my entire childhood in neurological terms.
Van der Kolk explains that the developing brain is extremely vulnerable to trauma. Before age seven, a child's brain is forming the neural pathways that will shape how they respond to stress, process emotions, and perceive safety for the rest of their life.
When trauma occurs during this critical window, it doesn't just create a bad memory. It becomes part of the brain's operating system.
Here's what that looked like for me:
My amygdala (fear centre) became overactive. I perceived threats everywhere—even when I was safe.
My prefrontal cortex (rational thinking) remained underdeveloped. I struggled to regulate emotions or think logically when I was triggered.
My hippocampus (memory processing) couldn't properly store the trauma. So instead of filing it away as "a scary thing that happened in the past," my brain kept treating it like it was happening NOW.
Translation: My nervous system was stuck in 1989, convinced I was still a four-year-old about to be hurt by people I trusted.

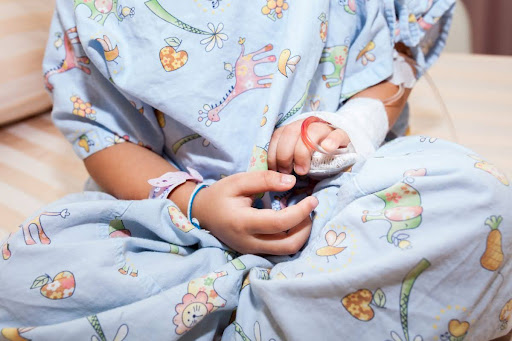
What Happens to a Child's Brain During Surgery
Let me paint the picture of what my brain was processing at age four:
I'm in pain. I don't understand why. Strange people are touching me, holding me down, hurting me. I'm screaming for my parents to make it stop.
But they don't.
They hand me over to these strangers. They walk away. And I'm left with people who are causing me pain.
To an adult brain, this makes sense: The doctors are fixing my hip. My parents trust them. This pain is temporary and necessary.
To a four-year-old brain? This is abandonment and betrayal.
Van der Kolk explains that young children lack the cognitive capacity to understand context. They can't rationalise that their parents are making a loving choice by allowing the surgery. All they know is: I'm terrified. I'm in pain. The people who are supposed to protect me aren't stopping this.
And when that experience happens during the years when your brain is forming its foundational beliefs about safety and trust?
Those beliefs get hardwired.
The Research on Early Medical Trauma
Here's what the research shows about trauma before age seven:
Brain development is disrupted. Studies have found that trauma significantly impacts a child's cognitive and emotional development. The younger the child, the more profound the impact.
Stress response systems get dysregulated. Children who experience medical trauma early develop hyperactive stress responses. Their bodies produce cortisol (stress hormone) constantly, even when there's no threat.
Attachment patterns are shaped. When children experience pain and fear without adequate comfort and protection, they learn that the world is unsafe and people can't be trusted.
Memory processing is impaired. Young children often can't form coherent narratives about their trauma. Instead, the trauma gets stored as fragmented sensory memories—sounds, smells, physical sensations—that trigger them without understanding why.
The American Medical Association Journal of Ethics highlights that Pediatric Medical Traumatic Stress (PMTS) is especially severe when it occurs during early childhood. Yet prevention and treatment remain woefully inadequate.
Research shows that trauma before age seven can lead to:
Difficulty regulating emotions
Chronic hypervigilance
Problems with trust and relationships
Physical health issues (IBS, chronic pain, autoimmune disorders)
Mental health challenges (depression, anxiety, PTSD)
All of which I experienced.

What This Looked Like in My Life
Let me show you how early surgical trauma shaped my brain and my life:
I Couldn't Regulate My Emotions
Remember the cupboard rage story I shared? Where I wanted to kill my mum over being told to close a cupboard?
That wasn't an anger problem. That was a four-year-old's trauma response firing in a 14-year-old's body.
Van der Kolk explains that when the brain's emotional regulation centres don't develop properly due to early trauma, people experience intense emotional swings they can't control. Zero to rage in seconds. Then crushing shame afterward.
That was my entire adolescence.
My Body Never Felt Safe
Chronic IBS. Insomnia. Sleep paralysis. Migraines. Unexplained pain.
All of these are documented responses to early childhood trauma. When your nervous system gets wired during fear, your body stays in a constant state of threat—even when you're safe.
Research shows that people with PTSD are 2.8 times more likely to have IBS. Up to 91% struggle with sleep disorders. The body literally keeps the score.
I Couldn't Trust Anyone
Relationships were nearly impossible for me. I pushed people away. I sabotaged good things. I expected abandonment because my brain learned at age four that even the people who love you most will hand you over to strangers who hurt you.
Logically, I knew my parents made the right choice. But logic doesn't override the wiring that gets installed before age seven.
I Kept Re-Traumatising Myself
Remember the hospital pattern? The bike crashes, bear chases, all the accidents that kept putting me back in the hospital?
Van der Kolk explains that trauma survivors often unconsciously re-create their trauma. Not because they want to suffer, but because familiar = safe to a traumatised brain.
My brain learned at age four that hospitals were "home." So when I felt overwhelmed emotionally, my unconscious would find ways to put me back there.
The Critical Window: Why Age Seven Matters
So why is age seven the cutoff?
According to developmental psychology and neuroscience research, age seven is roughly when the brain's foundational architecture is set.
Before age seven:
The brain is highly plastic (moldable)
Core beliefs about safety and trust are being formed
The nervous system is learning how to respond to stress
Memory processing systems are still developing
When trauma happens during this window, it shapes how all of these systems develop.
After age seven, the brain is more resilient. Trauma still impacts you, but it's less likely to fundamentally alter your brain's operating system.
This doesn't mean trauma after age seven isn't serious. It absolutely is. But trauma before age seven has unique developmental consequences because it happens when the foundation is being built.
I had my first surgery at four. Right in the middle of the most critical developmental window.
And no one told my parents that this could shape my brain for the next three decades.
What I Wish My Parents Had Known (And What You Can Do Now)
My parents did everything they could with the information they had. They were incredible. But here's what none of us knew back then—and what could have changed everything:
If Your Child Is Facing Surgery Before Age Seven:
1. Be present for the moments that shape their brain.
Waking up alone. Being moved into the hospital without you there. Crying at night with no immediate comfort.
These aren't just "difficult moments." These are experiences that tell a developing brain: You're alone. You have to cope with fear by yourself.
Be there when they wake up. Be there at night. Be there when they're scared and asking for you. Those moments matter more than anyone will tell you.
2. Get trauma-informed therapy immediately—not later.
Not when they start "acting out." Not five years down the line. Immediately after the surgery.
Early intervention can prevent PMTS from becoming lifelong PTSD. Find a therapist who specialises in pediatric medical trauma. Not all therapists understand how early surgical trauma impacts brain development.
3. Watch for signs of trauma (not character flaws).
When I came home withdrawn and unable to process emotions, my parents noticed. But no one connected it to the surgery.
Watch for:
Emotional dysregulation (intense emotions, difficulty calming down)
Withdrawal or sudden clinginess
Sleep problems, nightmares
Physical symptoms (stomach aches, headaches)
Regression (acting younger than their age)
Re-enacting the trauma in play
Avoidance of anything related to hospitals or doctors
These are trauma responses—not bad behavior. If you see them, get help early.
4. Help them create a narrative about what happened.
Young children need help making sense of their trauma. Without that, the trauma stays fragmented and terrifying—locked in the body as fear instead of as a coherent story with a beginning, middle, and end.
Talk to them about what happened in age-appropriate ways. Help them understand that the doctors were trying to help, not hurt. That their body is safe now. That what happened is over.

If Your Child Already Had Surgery Before Age Seven:
It's not too late.
Even if the surgery happened years ago. Even if you're just now realising this could be medical trauma. Even if they're teenagers or adults now.
It's not too late to help them.
Get them connected to a trauma-informed therapist. Help them understand that their struggles aren't character flaws—they're brain responses to early trauma. Give them language for what they're experiencing.
And be patient with yourself. You did the best you could with the information you had.
Just like my parents did.
The Full Story Is in the Book
What I've shared here is just a glimpse of how surgery before age seven shaped my brain and my life.
The full story includes:
The specific moments during surgery that created lasting trauma
How my parents' absence during key times reinforced core wounds
The decades of self-destruction that followed
The neuroscience of why my brain kept putting me in danger
The tools that finally helped me rewire my nervous system
I'm writing it all down because I know I'm not the only one living with the aftermath of early medical trauma.
Want to read the full story?
Join the book launch team and get:
✅ Free advanced copy (you'll read it before anyone else)
✅Exclusive 50% offon the print version so your Amazon review shows as "verified purchase" (Just $9.99)
✅ Behind-the-scenes access to the campaign + live Q&A sessions
✅ Early review instructions (yes—you can post your review even before you finish reading!)
✅ Virtual launch party invitation (celebrate with us!)
✅ The deep satisfaction of knowing your voice is helping someone else find healing, hope, and the truth that they're not alone
This isn't just about reading a book early. It's about being part of a movement to make medical trauma part of the conversation.
[Join the Launch Team - Link]
The Bottom Line
Surgery before age seven doesn't just create a difficult memory.
It shapes how your brain develops. How your nervous system responds to stress. How you process emotions. How you perceive safety and trust.
I spent 30 years thinking I was broken because I couldn't regulate my emotions, trust people, or feel safe in my own body.
Turns out, my brain was doing exactly what trauma brains do when the wiring gets installed during fear.
If you had surgery before age seven—or if your child did—you're not broken.
Your brain is responding exactly as it was designed to, based on what it learned during the most critical developmental window.
And with the right support, you can rewire it.
Kim
Related Posts:
[What Happens When ONE Doctor Speaks Up About Childhood Medical Trauma]
[Trauma Patterns You Can't See But Keep Putting You Back in Hospital]
Related Posts:
