
Child Facing Surgery? The 3 Moments Parents Must Not Miss
I don't remember my parents being at the hospital.
That's the brutal truth. Even though they were there. Even though they moved into the children's ward with me. Even though they took turns sleeping in uncomfortable chairs and advocating for me with doctors and doing everything humanly possible to help me through it.
I don't remember them.
What I do remember: Waking up alone. Crying alone. The peacocks that wandered into the ward with their tail feathers out (yes, this actually happened). The snack cart. The other kids. Kind nurses.
But my parents? Only two memories of their faces during the entire stay.
And it wasn't because they weren't there. It was because they weren't there at the moments when I needed them most.
Before I Go Further: This Isn't About Blame
I need to say this upfront because it's important.
My parents were incredible. They did everything they could with the information they had. They were dealing with their own stress, their own fear of watching their 4-year-old go through experimental hip surgery. They were trying to manage my older sibling at home. They were doing their absolute best.
And I love them for it.
This article isn't about what they did wrong. It's about what none of us knew back then—and what I hope other parents can learn now.
Because here's the thing: Pediatric Medical Traumatic Stress (PMTS) is real, and almost no one warns parents about it.
Research shows that trauma before age 7 significantly impacts a child's development, often causing lasting health and psychological challenges. Early hospitalizations disrupt cognitive and emotional development because young children need secure environments with consistent caregivers to thrive.
Hospitals? They're the opposite of that.
And yet, doctors rarely mention the psychological impact. They focus on the physical recovery—which makes sense, that's their job. But the emotional fallout? That gets missed.
So let me tell you what I wish my parents had known.
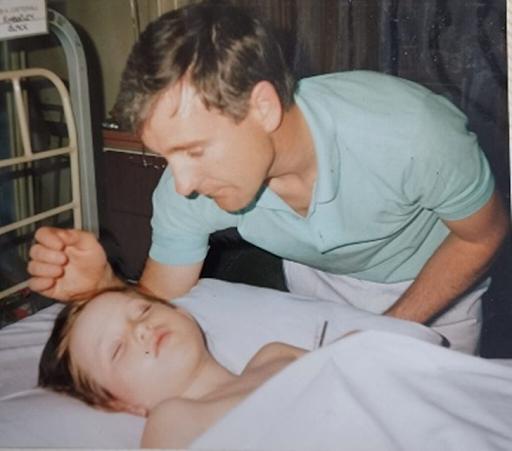
What Happened After My Surgery (That No One Warned Us About)
I was 4 years old when I had experimental hip dysplasia surgery. I spent my 5th birthday in the children's ward.
The physical recovery went well. The surgery was successful. I healed.
But emotionally? I came home a different kid.
My parents noticed it right away. I couldn't process emotions anymore. I withdrew from them. I went quiet in ways that felt different from normal childhood quietness.
But no one connected it to the surgery. How could they? No one told us this could happen.
By adolescence, I'd spiralled into drug use, violence, and alcohol abuse. I harboured rage toward my parents that lasted nearly a decade. Despite knowing deep down that I had a good upbringing, I was consumed by darkness I couldn't explain—shame, self-hatred, aggression.
It took 30 years to get a PTSD diagnosis from those childhood surgeries.
Thirty years of thinking I was broken. That something was fundamentally wrong with me. That I was weak for not being able to "just get over it."
All because no one warned us that surgery doesn't just traumatise the body—it traumatises the mind.
What Actually Causes Pediatric Medical Trauma
Here's what happens to a child during surgery:
They're in pain. They're confused. They're being handed over to strangers who hurt them (even though they're trying to help). They don't understand why their parents aren't stopping it.
To a child's developing brain, this feels like abandonment.
Their limited cognitive development prevents them from understanding context. They can't rationalise that "Mummy and Daddy let the doctors hurt me because it will help me walk." All they know is: I'm in pain. I'm scared. Where are my parents?
The American Medical Association Journal of Ethics highlights that children experience significant psychological distress during hospital stays and medical procedures. This often leads to Pediatric Medical Traumatic Stress—emotional and physical responses to pain, injury, illness, and invasive medical experiences.
The journal emphasises that clinicians have an ethical responsibility to use trauma-informed care practices to reduce psychological harm. But here's the problem: that responsibility often ends when the child is discharged.
Once you go home, you're on your own.
And as medical advancements improve survival rates for pediatric conditions, PMTS cases are expected to rise. Yet research on prevention and treatment remains limited.
Translation: More kids are surviving surgeries, but we're not preparing families for the emotional aftermath.

The 3 Moments That Matter Most
After years of therapy and deep conversations with my mum about what happened during my hospital stay, we identified three critical moments when parental presence makes the biggest difference.
These aren't the only moments that matter. But they're the ones that shaped my trauma—and the ones I remember most vividly.
Moment #1: Mornings Matter More Than You Think
Mornings are when children are most vulnerable.
When you wake up, your brain is assessing your surroundings: Am I safe? Where am I? Who's here?
For a child in a hospital, waking up alone triggers fear. Even if you arrive ten minutes later, those ten minutes shape how safe they feel.
During my hospital stay, my mum often arrived after I'd woken up and eaten breakfast. I asked her to come earlier—to be there when I opened my eyes.
She didn't.
Not because she didn't care. But because she was juggling so much and didn't realize how much it mattered.
She regrets that decision to this day.
And I don't blame her. How could she have known? No one told her that mornings were critical. No one explained that a child waking up alone in a hospital internalizes that as: I'm not important enough for them to be here.
That's not logical. But trauma isn't logical.
If your child is hospitalized, be there when they wake up. Even if it's hard. Even if it means sleeping in an uncomfortable chair. Those first moments of consciousness set the tone for their entire day.
Moment #2: Nighttime Is When Fear Lives
Bedtime and nighttime are equally critical.
This is when children are most scared. The hospital is dark. Sounds are amplified. Their imagination runs wild. And if they wake up in the middle of the night in pain or fear, they need to know someone is there.
After I was discharged, I slept downstairs alone because my parents were worried about carrying me upstairs while I was in a brace. I woke up constantly—crying, itchy, uncomfortable, distressed.
No one came immediately. I had to cry loud enough and long enough for someone upstairs to hear me.
That felt like abandonment.
Again—not because my parents didn't care. But because they didn't know how much it mattered.
Eventually, my grandmother decided to sleep in the same room as me. And suddenly? I slept through the night. I felt safe. My distress stopped.
My parents finally got rest too.
If possible, sleep in the same room as your child during recovery. I know that's a big ask. I know you're exhausted. But their sense of safety depends on knowing you're close.
Moment #3: When Your Child Asks for You, They Need You
Children don't always have the words to explain what they need.
But if they're asking for your presence—if they're saying "please stay" or "don't leave" or "come earlier"—it's because they need you.
Not want. Need.
Surgery makes a child feel powerless. Their body has been violated (even though it's for their own good). They've endured pain they don't understand. The only thing that makes them feel safe is you.
When you're not there during key moments, their brain files it as: I'm alone. I have to cope with this by myself. I can't trust anyone to protect me.
That becomes a core belief that shapes how they see themselves and the world.
Listen to your child's requests. Evaluate whether it's a deep need or a surface-level want. Some moments that seem small to you—like being there when they wake up—might be terrifying to their underdeveloped mind.

What My Parents Missed (And What It Cost Me)
There are moments from my hospital stay that I remember vividly.
Being moved into the hospital. The sensation of it. The fear. My parents weren't there for that.
Waking up alone, already having eaten breakfast, waiting for someone to show up. Feeling forgotten.
Crying downstairs at night, unable to move, waiting for someone to hear me.
None of these were my parents' fault. They were doing their best. But because no one warned them that these moments mattered, I processed them as abandonment.
And that abandonment became the foundation for 30 years of PTSD.
Emotional numbness. Aggression. Recklessness. Inability to trust. Rage at the people who loved me most.
I don't want that for your child.
Here's the Hope: You Can Prevent This
If your child is facing surgery, you have a chance to do what my parents didn't know they needed to do.
You can be there for the moments that matter most.
You can't prevent the surgery. You can't take away the pain. But you can be present in ways that signal to your child's developing brain: You are safe. You are loved. You are not alone.
That presence—especially in the mornings, at night, and when they ask for you—can be the difference between trauma that heals and trauma that lasts a lifetime.
I want to be clear: Even if your child does develop PMTS, it's not the end of the world.
My experiences haven't been solely detrimental. I've become fiercely independent, resilient, and self-aware. I live life on my terms. I face challenges head-on. I'm proud of the woman I am today.
But I also spent 30 years suffering unnecessarily.
And if I can help even one family avoid that, it's worth sharing my story.
To the Parents Reading This
If your child is in the hospital right now, hang in there.
You are the most important person in their life. They are lucky to have you by their bedside.
I can only imagine the strength it takes to watch your child go through surgery. I love my parents. I'm grateful they agreed to the surgery—because today, I can walk and run. They did the best they could with what they had.
And that's all I could have ever asked for.
My goal in sharing this isn't to make you feel guilty or scared. It's to give you information that wasn't available to my parents.
Pediatric Medical Traumatic Stress is real. It affects up to 80% of hospitalised children. And it's preventable—if you know what to look for and when your presence matters most.
Be there in the mornings. Be there at night. Listen when your child asks for you.
Those small moments? They're everything.
Want to Learn More About Childhood Medical Trauma?
My book (launching May 2026) includes a full chapter on my childhood surgeries and how undiagnosed PTSD shaped my life for 30 years.
Join the launch team and get:
✅ Free advanced copy (you'll read it before anyone else)
✅ Exclusive 50% off on the print version so your Amazon review shows as "verified purchase" (Just $9.99)
✅ Behind-the-scenes access to the campaign + live Q&A sessions
✅ Early review instructions (yes—you can post your review even before you finish reading!)
✅ Virtual launch party invitation (celebrate with us!)
✅ The deep satisfaction of knowing your voice is helping someone else find healing, hope, and the truth that they're not alone
This isn't just about reading a book early. It's about being part of a movement to make medical trauma part of the conversation.
[Join the Launch Team - Link]
Related Posts:
[What Happens When ONE Doctor Speaks Up About Childhood Medical Trauma]
[7 Signs You Have Medical PTSD (That Your Doctor Never Mentioned)]
[Abigail's Story: How One Doctor's Warning Changed Everything]
Cited Articles & Resources
Centers for Disease Control and Prevention (CDC). (2024, May 16). About adverse childhood experiences. Adverse Childhood Experiences (ACEs). https://www.cdc.gov/aces/about/index.html
Christian‐Brandt, A. S., Santacrose, D. E., Farnsworth, H. R., & MacDougall, K. A. (2019). When treatment is traumatic: An empirical review of interventions for pediatric medical traumatic stress. American Journal of Community Psychology, 64(3-4), 389-404. https://doi.org/10.1002/ajcp.12392
Kassam-Adams, PhD, N., & Butler, MD, L. (2017). What do clinicians caring for children need to know about pediatric medical traumatic stress and the ethics of trauma-informed approaches? AMA Journal of Ethics, 19(8), 793-801. https://doi.org/10.1001/journalofethics.2017.19.8.pfor1-1708
Kolk, B. V. (2014). The body keeps the score: Brain, mind, and body in the healing of trauma. Penguin UK.
Marsac, M. L., Kassam-Adams, N., Delahanty, D. L., F. Widaman, K., & Barakat, L. P. (2014). Posttraumatic stress following acute medical trauma in children: A proposed model of bio-psycho-Social processes during the Peri-trauma period. Clinical Child and Family Psychology Review, 17(4), 399-411. https://doi.org/10.1007/s10567-014-0174-2
